| MEDICAL INTRO |
| BOOKS ON OLD MEDICAL TREATMENTS AND REMEDIES |
THE PRACTICAL |
ALCOHOL AND THE HUMAN BODY In fact alcohol was known to be a poison, and considered quite dangerous. Something modern medicine now agrees with. This was known circa 1907. A very impressive scientific book on the subject. |
DISEASES OF THE SKIN is a massive book on skin diseases from 1914. Don't be feint hearted though, it's loaded with photos that I found disturbing. |
OTHER ANIMAL PARASITES, OF MINOR IMPORTANCE, PENE
TRATING THE SKIN
Leptus (harvest bug; mower’s mite; Fr., Rouget; Ger., Erntemilbe), of which
several varieties (leptus autumnalis, leptus Americanus, leptus irritans), with but
slight minor differences, are encountered, is a minute, barely macroscopically visible
parasite, elongate, pyriförm, or ovalish in shape, of an orange-red or brick-red color,
and with six long legs. It is found in summer in harvest-fields, in grass, bushes, in
swampy regions, and along the river-banks. It buries itself partly or more or less com
pletely in the skin, and gives rise to a good deal of irritation, which may be of an ery-
thematous, urticarial, papular, vesicular, or pustular aspect, and when several or more
are close together, may present an eczematous appearance. The lower extremities,
especially about the ankles and feet, are the favorite parts, although other regions, such
as the hands and arms, are sometimes invaded. One variety (leptus Americanus),
according to Duhring, is found in the axillae and scalp, as well as other parts of the
body, and more frequently in children.
Treatment consists in the application of weak ointments of sulphur, balsam of
Peru, and other parasiticides. A carbolized boric acid lotion is also useful.
Pulex penetrans (rhinochoprion; chigoe; chigger; jigger; sand-flea; Fr., puce de
sable; chique; Ger., Sandfloh) is an almost microscopic parasite, especially of warm and
tropical climates, which in its general features resembles the common flea, except that
it is furnished with a long proboscis. The impregnated female, which alone is the inva
der, penetrates and burrows into the skin, producing an inflammatory swelling, vesicle,
pustule, abscess, or even ulceration. The feet, especially the toes, are the favorite
sites of attack, particularly alongside or just under the nail. Other parts are some
times invaded, as the knee, scrotum, back, etc The parasite sometimes gives rise to
considerable disturbance, with adenitis.
Treatment consists in the removal of the parasite and applications to relieve the
irritation. The former is accomplished by careful extraction, usually with a blunt
needle, and the latter by means of carbolized boric acid or alkaline lotions. If the
more severe conditions are provoked, these are treated upon general principles. Essen
tial oils are commonly used as a protection against the parasites.
Dracunculus1 (dracunculus medinensis; guinea-worm; guinea-worm disease;
dracontiasis; filaria medinensis; Fr., ver de Guinée; dragonneau; filaire de Médine; Ger.,
Peitschenwurm; Medinawurm).—This parasitic nematode worm is found in tropical
countries, especially in upper Egypt, Persia, India, west coast of Africa, Senega, Guinea,
1 Some important general literature: Horton, Guinea-worm or Dracunculus, London,
1868; Leuckart, Die Menschlichen Parasiten, 1876, vol. ii; Manson, “On the Guinea
Worm,” Brit. Med. Jour., 1895, ii, p. 1350; Dubreuilh and Beille, “La filaire de Médine,”
Arch, clinique de Bordeaux, 1897, p. 425 (with résumé and references).
1196
PARASITIC AFFECTIONS
etc When matured, the female, which is the invader, attains from one to several feet
in length, averaging about 25 inches, and is about 1/15 to 1/10 inch in thickness, being some
what flattened. It has a slightly convex head and a curved and pointed tail, and is of a
milky color. It was formerly thought that it gained entrance in various ways, but it is
now known (Fedschenko, Stambolski, Forbes) that the embryos which enter the water
gain access to a minute crustacean (cyclops) and undergo larval development, the
crustaceans finding their way to man through the drinking-water. The larvæ escape,
develop, and the female begins to migrate into the tissues, where it remains, giving
rise to no trouble until fully developed. Its migrations may then continue for some
months, and even after its appearance near the surface is noted may sometimes continue
its travels before it finally seeks exit. At the point where it appears it may present a
cord-like appearance under the skin, and in other instances it can be felt as a worm or
cord-like mass. Usually, however, the first sign is a local inflammation, developing into
a vesicopustular, nodular, or boil-like formation, attended with more or less pain and
swelling. This breaks, and at the bottom of the cavity the head of the worm is seen.
Through this opening the worm may, with its contained young, gradually be extruded;
or it may, if disturbed, or voluntarily, be withdrawn, the opening close up, and a new
formation appear elsewhere, usually near by, where it again attempts to find exit.
The rupture of the worm, the escape of the embryos into the tissues, and the severance
of the head in attempts to dislodge the parasite, leaving the worm in the tissues, are
variously stated to be fraught with some danger, such as the development of lymphan
gitis, gangrene, septicemic symptoms, and death. Sometimes the parasite is destroyed
by the suppurative inflammation which may be excited, and with possible untoward
consequences. The part at which the worm is commonly seen is the foot, not infre
quently on the thigh, occasionally on the hands and elsewhere. In most instances
there is but one worm, although two are sometimes present, and exceptionally they
may exist in numbers.
In regions where the malady is endemic the appearance of a local inflammatory,
boil-like swelling might be suggestive, but no positive diagnosis can be made until the
worm can be felt or seen.
Treatment practised by the natives in endemic regions consists in securing the
protruding head part, and gradually, day by day, winding the worm with gentle trac
tion around some substance until it is all withdrawn, ceasing traction each time that
the parasite makes opposition. Perrin1 states that plunging the part into cold water
hastens this process, the parasite temporarily relaxing its hold. This method is, how
ever, unscientific, slow, not without danger, and takes many days. According to
Forbes, if the worm is let alone it emerges spontaneously in from fifteen to twenty days
from her first appearance. The plan which promises well is that by Emily,2 of injecting
into the forming tumor a solution of corrosive sublimate (1 : 1000); if the head has al
ready protruded, he injects the solution into the body of the worm. This method has
since been successfully used by Davoren,3 Blin,4 Manson and Boyd.5 As Manson suc
cinctly states, a “dead aseptic guinea-worm does not act as an irritant to the tissues,
and it can be got rid of by absorption like any aseptic animal ligature.” The method
advocated by Horton has been effective, consisting of the administration of moderate
to large doses of asafetida. Tilbury Fox and others reported success with this plan, the
parasite, which the remedy seems to destroy, either being gradually discharged or re
maining in the tissues, becoming encysted or slowly absorbed. Forbes states that sul
phur internally is likewise efficient.
1 Perrin, Annales, 1896, p. 1315.
2 Emily, Arch, de méd. navale, 1894, No. 6, vol. lxi, p. 460.
3 Davoren, Brit. Med. Jour., Oct. 17, 1894.
4 Blin, Arch, de méd. navale, Nov., 1895, No. 5, vol. lxiv, p. 368.
5Manson and Boyd, Brit. Jour. Derm., 1896, p. 37.
DEMODEX FOLL1CULORUM
1197
Cysticercus Cellulosœ.—Our first knowledge of the presence of the cysticercus of
tænia solium in the subcutaneous tissues we owe to Rokitansky.1 According to
Küchenmeister and Zurn, the proportion of integumental infection compared to that
of other organs is about 5 per cent., which Geber2 considers a rather low estimate.
The malady is most frequently encountered in North Germany, where raw or half-
cooked pork is a favorite article of diet. The tumor caused by its presence is situated
under rather than in the skin, and varies in size from a large pea to that of a walnut,
the larger formation dependent upon the reactive inflammation excited. There may
be several or many. They are ordinarily not sensitive to pressure unless from reac
tionary inflammation, although at times they may be spontaneously painful. The
integumental covering rarely shows any change. In shape they are rounded or ovalish,
smooth and elastic, or even firm and hard, and, as a rule, more or less movable. After
reaching a variable size they may remain stationary somewhat indefinitely, although
after death of the parasite they become smaller and exhibit a tendency to calcification.
The trunk is a favorite locality, likewise the extremities, and occasionally they are seen
on other parts.3
Their chief interest lies in the diagnosis, as the tumors bear some resemblance to
other growths, and, in fact, a positive conclusion is, as a rule, possible only by micro
scopic examination, which reveals the presence of the cysticerci. Examination of the
contents, obtained by puncturing, usually suffices, as the hooklets are easily found in
the discharge.
Demodex folliculorum (acarus folliculorum; steatozoon folliculorum; entozoon
folliculorum; Fr., acare des follicules; Ger., Haarbalgmilbe) is a minute, microscopic

Fig. 322.—Demodex folliculorum (ventral surface; X 300) (after Simon).
parasite, found in the sebaceous glands and hair-follicles, the first knowledge of which
we owe to Henle (1841) and Simon (1842). It has most commonly an elongated, worm-
like form, made up of a head, thorax, and long abdomen, with eight short stout legs
coming off from the thorax; the larva has but six legs. The parasite varies in length
considerably, some being quite short. It is present most abundantly in the sebaceous
glands and hair-follicles of the nose, forehead, and cheeks, and is easily found in the
pressed-out sebaceous matter. It seldom occurs in infants (Duhring) nor in all adults,
but is most frequently to be seen in greatest numbers in those of thick, greasy skin.4
1 G. Lewin, “Ueber Cysticercus cellulosæ in der Haut des Menschen,” Archiv, 1894,
vol. xxvi, pp. 70 and 217 (gives complete exposition with review of the literature and
references).
2 Geber, Ziemssen`s Handbook of Skin Diseases, p. 549.
3 Pye-Smith, Brit. Jour. Derm., 1892, p. 366, had a case under observation with
more than 50 tumors scattered over face, neck, trunk, and limbs; they were quite pain
less; their true nature was not suspected until the microscope cleared the matter up.
4 Gmeiner, Archiv, 1908. vol. xcii, p. 25 (with several plates), gives a good historical
summary and description of the morphology of the demodex folliculorum; investigation
was made with 200 corpses, and with the exception of infants the parasite could be
found on the face of every individual; DuBois (“Recherches sur Demodex folliculorum
hominis dans la peau same,” Annales, 1910, p. 188), in a large series of examinations on
living subjects found it absent in those under the age of five; it or its larva present in
50 per cent, of the subjects, between five and ten, and present in all above ten; eggs of
the parasite develop into hexapod larval forms.
1198 PARASITIC AFFECTIONS
It has been thought to be harmless, but recently De Amicis,1 Majocchi2 (2 cases),
and Dubreuilh3 have reported instances of pigmentation involving parts of the face due
to its presence, the pigmentation being of a fawn or brownish tint, similar to that of
tinea versicolor. In Dubreuilh’s patient the neck was also the seat of the discoloration,
and some spots were found on the breast. The chin and lip regions are apparently favor
ite situations. There was slight, but scarcely perceptible, follicular prominence, due
to minute corneous projections from the orifices, associated with, in one or two instances,
trifling scurfiness. Dubreuilh noted that the pigmentation started and was most
pronounced about the follicular outlet. The clinical appearances suggested tinea versi-
color to these observers, but upon microscopic examination the fungus of this disease
was not found, but the demodex was discovered in numbers, and this was noticeable only
in the pigmented parts. It is well known, of course, that other or allied varieties of this
parasite are found in some of the lower animals, and in which it may be productive of
considerable mischief.
The treatment in De Amicis’ case, which was successful, was by washings with soft
soap. Dubreuilh tried a stimulating parasiticide application, but without any result
ing benefit.
Œstrus (Gad-fly; Bot-fly).—The larvae of both the families of the muscidæ and
œstridæ4 are occasionally found invading the human skin, although there is none pecu
liar to man. Such invasion, especially by the latter, is not uncommon in Central and
South America, and is also met with exceptionally elsewhere. The ova of the former
are deposited usually in open wounds and ulcers, sometimes creating serious trouble,
and naturally come more under the surgeon’s observation. The ova of the œstridæ
are deposited in the skin in the puncture made by the insect, most frequently on ex
posed parts, the larvæ developing and giving rise to furuncle-like tumors. These for
mations generally have a central aperture through which a sanious, seropurulent, or
sanguinopurulent fluid exudes. In some instances, as the result of burrowing of the
worm, irregular lines resembling inflamed lymphatics, of a purplish or purplish-red
color, are produced. In rare cases considerable surface may be traversed by the larva
before final suppurative action is excited, an abscess-like tumor formed, and the worm
can be pressed out or extracted.5
The treatment of the formation produced by the œstrus consists in the removal
of the parasite by free excision and pressure, and application of antiseptics to the
1 De Amicis, “Demodex folliculorum e ipecromia cutanea,” Giorn. ital., 1898, p.
205—brief abs. in Brit. Jour. Derm., 1899, p. 42.
2Majocchi, ibid.
3 Dubreuilh, “Pigmentation cutanée causée par le demodex folliculorum,” Jour, de
méd. de Bordeaux, No. 4, Jan. 27, 1901.
4 See exhaustive paper by G. Joseph, “Ueber Myiasis externa dermatosa,” Monats-
hefte, 1877, pp. 49, 106, and 158, with review of the whole subject and literature refer
ences. Joseph places the cutaneous malady variously produced by the different species
under the above name; subdividing the cases into two classes: those due to the family
muscidæ, myiasis dermatosa muscosa, and those due to the œstridæ, myiasis dermatosa
œstrosa; also that by Strauch, “Myiasis Dermatosa,” Jour. Cutan. Dis., 1906, p. 524
(with some references); Yount and Sudler, “Human Myiasis from the Screw-worm Fly,”
Jour. Amer. Med. Assoc, 1907, vol. xlix, p. 1912, chiefly intranasal, and in the south
and southwest; Gilbert, Archives Int. Med., 1908, vol. il, p. 226; Miller, Jour. Amer.
Med. Assoc., Dec 3, 1910, gives notes of a case of “Myiasis Dermatosa due to the Ox-
warble Flies”; it occurred in a white boy aged eleven, and presented itself as a traveling
“lump.” The lumps were occasionally stationary, but generally migrated 3 to 4
inches a day. The larva, according to examination by C. W. Stiles, was identified as
“the larva of hypoderma lineata in the second stage”; a somewhat similar case is referred
to: Kane, “Insect Life,” ii, 238, traveling lump, finally breaking down, and found due to
the larva of the hypoderma bovis.
5 McCalman, Brit. Med. Jour., 1879, vol. ii, p. 92, and Arch. Derm., 1880, p. 174;
W. G. Smith, Trans. Internat. Cong., London, 1881, vol. iii, p. 181, and abs. in Arch.
Derm., 1882, p. 45; and Walker, Brit. Med. Jour., 1870, vol. i, p. 151, report interesting
examples.
CREEPING ERUPTION
1199
lesion and wound thus made. In the more conspicuous serpiginous cases the larva
can sometimes be secured by excision of an area around or just beyond the advancing
part.1
Creeping eruption (Lee),2 also named larva migrans (Crocker), hyponomoderma
1 Foster (“Gastrophilus Epilepsalis Larvæ in the Skin of an Infant,” St. Paul Med.
Jour., Oct., 1903) records a case of an infant three weeks old, with a papular and pustu
lar eruption on the neck, a pustule on the palm, and one between the great and second
toes of right foot, of a few days’ duration; from three lesions of which (the one between
the toes, the one on the back of the neck—somewhat nodular or furunculoid—and the
one in the palm) a small living worm came out. The worms were about 1/5 inch in length,
and evidently the larvæ of some species of fly—later identified by Coquillet as gas-
trophilus epilepsalis, a species somewhat closely allied to gastrophilus equi or bot-fly.
Vignolo-Lutati (Archiv, 1907, vol. lxxxvii, p. 81) described, under the title “Oxy-
uriasis cutanes,” a case of acute seropurulent dermatitis of the peri-anal and genitocrural
regions in a man aged twenty-four, the most inflamed skin being dotted over with
vesicopustules, due to the presence and colonization of the oxyuris vermicularis in the
skin of the peri-anal region; the worms were detected in large numbers in the discharge.
He refers to several similar cases (Szerlecky, 1874; Michelson, 1877; and Majocchi,
1893).
Spoor (“Infection with Fly Larvæ,” Jour. Amer. Med. Assoc, 1907, vol. xlix, p.
1775) saw in an infant four weeks old several lesions about the neck and face, forearms,
and hands; some slightly raised, with a red areola around a whitish center of seropuru-
lent material about the size of a pin-head, from which a “worm” escaped when the lesion
was pressed between the fingers, as one would extract a comedo—afterward healing
taking place rapidly. There were also larger lesions (one as large as a plum), represent
ing a more severe type of inflammation, and contained larger larvæ. The larvæ varied
in size, and microscopically resembled somewhat the small worm found in apples.
Stiles (“The Occurrence of a Proliferating Cestode Larva (Sparganum proliferum)
in Man in Florida,” Jour. Cutan. Dis., 1908, p. 345, with illustrations) records (Gates’
patient) a case where numerous cystic nodules in the skin and in the fascia between the
skin and muscles were scattered over the trunk, and of long duration. When opened
the lesions were found to contain one to three worms about 1/16 inch wide and 5/8 inch
long; the most striking feature of the worm being its irregular shape, with tendency to
proliferation by forming supernumerary heads. Stiles also reviews an apparently simi
lar case (Ijima’s Japanese case).
Costa (“Two Important Parasites of the Skin,” Jour. Cutan. Dis., Jan., 1910) re
cords a case in a child where several rather large tumefactions on the head were due to
the presence of a worm, probably the larva of an œstride, the dermatobia noxialis. The
other parasite to which he calls attention is the sarcopsylla penetrans, which penetrates
the skin of the feet, producing a variable degree and type of inflammation.
2 Lee, “Creeping Eruption,” London Clin. Soc’y Trans., 1874, vol. viii, p. 44, and
ibid., 1884, vol. xvii, p. 74; Crocker, “Larva migrans,” Diseases of the Skin, second
edit., p. 926; Neumann, “Ueber eine neue Hautaffection,” Verhandl. des V. Cong. d.
Deutschen dermat. Gesellsch., 1895 (1896), p. 95; Sokolow, “Ueber eine Würmchen,
welches in der epidermoidalen Schichte der menschlichen Haut Gänge bildet”—abs. in
Archiv, 1897, vol. xxxviii, p. 153; Samson-Himmelstjerna, “Ein Hautmaulwurf,” ibid.,
1897, vol. xli, p. 367; Kumberg, “Ein Fall von Dermatomycosis linearis migrans
œstrosa”—abs. in Dermatolog. Centralbl., 1897-98, vol. i, p. 283; Kaposi, Wiener klin.
Wochenschr., 1898, p. 399 (case demonstration); Van Harlingen, “Report of Three
Cases of Creeping Larvæ in the Human Skin” (Hyponomoderma, Kaposi), Amer. Jour.
Med. Sci., September, 1902; Stelwagon, “A Case of Creeping Eruption,” Trans. Section
of Cutaneous Medicine and Surgery of the A. M. A. for 1903, and Jour. Cutan. Dis.y
1903, p. 502; “A Second Case of Creeping Eruption,” Jour. Cutan. Dis., 1904, pp. 359,
381 (each with illustration); Hamburger, “Creeping Eruption; Its Relations to Myiasis,”
Jour. Cutan. Dis., 1904, p. 217; Shelmire, “Creeping Eruption; Report of a Case,”
ibid., June, 1905 (on a finger of a physician); Hutchins, ibid., 1906, p. 270 (2 cases;
successful treatment by injection of a drop or two of chloroform); Moorhead, Texas Med.
News, February, 1906 (cure in 5 cases by freezing the advancing end with ethyl chlorid);
Kengsep, Dermatolog. Centralbl., April, 1906, p. 194 (1 case, with résumé); Hutchins
(third case), Jour. Cutan. Dis., 1908, p. 521; Wosstrikow and Bogrow (“Zur Ætiologie
der ‘Creeping Disease,’" Archiv, 1908, vol. xc, p. 323, plate illustrations) have met with
2 or 3 cases yearly for the past twenty years, but never able to discover the parasite till
in a recent case; it consisted of a minute (1 mm.) worm with blackish head and white
body, with active wave-like movements, and, according to Prof. Koschewnikow, it is
an immature gastrophilus larva, probably of the gastrophilus hæmorrhoidalis of the
horse; Gosman, Jour. Amer. Med. Assoc, Jan. 1,1910, p. 38 (2 cases; 1 with two sepa-
I200
PARASITIC AFFECTIONS
(Kaposi), and dermamyiasis linearis migrans œstrosa (Kumberg), is a curious malady,
first described by Lee, Crocker, and subsequently by others, and has the peculiar fea
ture of traversing the surface, as the name signifies. The burrow made by the parasite
is 1/8 to 1/6 inch in diameter, and, at least in its extending part, just perceptibly raised,
and of a pale rose-pink or reddish color. In the part less recently traversed the line is
sometimes a thin, elevated, more or less continuous, broken or bead-like linear vesicle
(as in the appended illustration); this in the still older part dries into a thin crust.
Sometimes the whole line is merely a slightly raised erythematous thread-like formation,
most pronounced at its extending part, and fading away at the older traversed part.
The parasite travels at the rate of a fraction
of an inch to several inches daily and seems
more active during the night—in Haase’s
case it was noted only at this time. It may
take a tortuous, irregular, or erratic course,
and even traverse a great part of the body.
Exceptionally, there is more than one parasite
present (rarely more than two), as in one of
my cases, giving rise, to a similar correspond
ing extending burrow. The formation is due
to a minute migrating larva, which Sokolow,
Samson-Himmelstjerna, and Rudell have
found. According to Samson it is more
readily detected by pressing the blood out of
the part by means of a flat piece of glass,
through which, with the aid of a magnifying
lens, the parasite can be seen as a black
speck. In one of my cases I was able—and
Rudell also—to corroborate this, but I did
not succeed in getting possession of the para
site. Rudell succeeded by making a small
flap-like incision, with a small cataract knife,
directly in front of the dark speck; on lifting
the flap the larva emerged from its burrow.
This malady is met with most commonly
in Southern Russia; it is rare with us, but
during the last several years cases have been
recorded, in the order named, by Van Har-
lingen, myself, Hamburger, Shelmire, and
others. In almost all cases the starting-point
of the lesion is on those parts most exposed to inoculation and invasion—hands or
lower part of the forearm, the feet or lower part of the leg, and the buttocks or adjacent
part of the back. In all of my 4 cases, and also in some instances reported by others,
the malady began at or after a visit to the sea or seashore. According to Sokolow, the
parasite, resembling the larva of a fly, is 1 mm. in length, with ten segments, and hook-
lets, with, at the headend apparently, two suckers; he considered it the larva of a
bot-fly, or œstreus, of the genus Gastrophilus, probably of the species hæmorrhoidal.
It was also stated by this observer that black nits could be found adherent to the hairs
in the neighborhood of the burrow.
Treatment usually advised consisted in excising or cauterizing an area around or
just beyond the advancing part. In my cases I applied cataphoretically a solution of
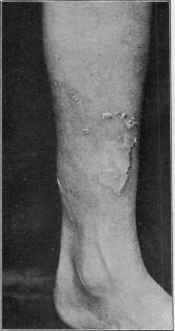
Fig. 323.—Creeping eruption (larva
migrans) in a youth aged eleven; there
was also an active extending burrow
on the back.
rate burrows); Haase, Jour. Cutan. Dis., 1910, p. 393 (1 case, two burrows, dorsum of
both feet; progress noted only during night; good case illustration); Rudell, Jour. Amer.
Med. Assoc., July 26, 1013 (2 cases, 1 with two burrows, one of which going over the
eyelid, crossing from the upper to the lower lid during the night; good illustration).
GROUND ITCH I20I
mercuric chlorid 2 grains to the ounce (0.13:32.) to a 11/2-inch area around the advancing
end of the burrow, and applied a minute quantity of nitric acid to the suspected site
of the parasite, just beyond the extreme end of the line; a magnifying glass should be
employed to discover this point, as it is slightly in advance of where it appears to be by
unaided vision. These cases were all cured within a week by this method, more
probably by the nitric acid than by the cataphoresis. Hutchins had marked success
with the injection of a few drops of chloroform.
Craw-craw is a malady observed chiefly on the west coast of Africa, having to
some extent the aspects of scabies, which is caused by nematodes, according to Nielly,1
a species of the genus Leptodera and family anguillulidæ, and in Corre’s and O’Neill’s2
opinion to a kind of filaria. The fingers and forearms are always predominantly, and
sometimes exclusively, affected. The eruption, as to be inferred from its resemblance
to scabies, consists of papules, vesicles, and pustules, discrete or crowded, and frequently
with considerable crusting, and is exceedingly itchy. There are no cuniculi, however,
as in scabies, nor the same peculiar distribution. The parasites in craw-craw can be
found in the scrapings and in the seropurulent liquid.
The disease is rebellious to treatment, consisting of thorough cleanliness, baths,
removal of the crusts, and sometimes the curetting-out of the underlying soft tissue,
together with the use of parasiticides.
The echinococcus larva, while usually found affecting the internal organs, excep
tionally gives rise (echinococcus cutis) to a softish, fluctuating, semitranslucent, pro
jecting tumor, somewhat larger than those of the cysticercus. It is seated in the sub
cutaneous tissue, and has been found more frequently in women. The covering in
tegument is unchanged. Encapsulation of the parasite takes place; it perishes in one
or two years, the tumor undergoing calcification. There are no subjective symptoms
except a sensation of tension and heaviness. According to Geber, the semitranslucent
character of the tumor, its superficial seat and projection without alteration of the skin,
and the fluctuation are the features of diagnostic value; supplemented by exploratory
incision and finding the hooklets of the parasite. Treatment consists of extirpation.
The distoma hepaticum, or liver-fluke, has, according to Küchenmeister, been
found in the subcutaneous tissues of human beings in three instances—one woman
and two men—giving rise to a tumor-like formation. In one the site was the region
of the ear, another the lower extremities, and the third the trunk. The subjective
symptoms varied, being practically nil, in one instance painful, suggestive of the pain
of a developing abscess. Diagnosis was possible only by finding the distoma.
Ground itch3 or uncinarial dermatitis, observed in certain tropical countries (also
called water-itch, water-pox, water-sores, sore feet of coolies, panighao; and in Porto
Rico, also, “mazamorro”), consists primarily of an erythematous or an erythemato-
papular and papulo-vesicular eruption of the feet due to the irritation of these parts
by the larvæ of the hookworm. Uncinariasis, ankylostomiasis, or hookworm disease
(also known as dochmiasis, tropical chlorosis), is, as known, a serious, and when un
treated, often fatal, constitutional malady characterized by depression of the vital
forces, profound anemia and inertia. It is due to the intestinal parasite (probably of
several varieties) known variously as uncinaria duodenalis, ankylostoma duodenalis,
1 Neilly, Bull, de l' acad. de med. de Paris, 1882, p. 395.
2 O’Neill, Lancet, 1875, i. P. 265.
3 Recent literature of Ground itch: Stiles, “The Significance of the Hookworm
Disease for the Texas Practitioner,” Trans. State Med. Assoc. of Texas, 1903, p. 353
(an excellent, clear, and complete exposition and review); C. A. Smith, “Remarks on
the Mode of Infection in Uncinariasis,” Jour. Amer. Med. Assoc, 1905, vol. xlv, p. 1142,
and ibid., 1906, vol. xlvii, p. 1693; Leonard, “Ankylostomiasis or Uncinariasis,” Jour.
Amer. Med. Assoc, 1905, vol. xlv, p. 588; Dubreuilh, “L’Ankylostomiase Cutanée,” La
Presse Méd., April 15, 1905; Ashford, “The Problem of Epidemic Uncinariasis in Porto
Rico,” Jour. Assoc. of Military Surgeons, Jan., 1907, p. 40. These various papers refer
to the observations of Looss, Sandwith, Bently, and others. Cole, “Necator Ameri-
canus in Natives of the Philippines,” Philippine Jour, of Sci., Manila, Aug., 1907.
76
1202 PARASITIC AFFECTIONS
dochmius duodenalis, uncinaria americana, necator americanus, and belonging to the
nematode family Strongylidæ (Stiles). It was formerly thought that the larvae of the
uncinaria found entrance by the mouth in food or water, but it is now known, through
the observations and experiments of Looss, Schaudinn, Sandwith and Smith, and others
that a common mode of entrance is by way of the skin of the lower extremities in those
going barefooted in moist or wet, muddy and sandy soil, the eggs of the parasites finding
their way here in the alvine discharges from affected persons. The cutaneous disturb
ance begins commonly as reddish spots or macules which soon show papulation or
vesicles; the latter may coalesce and form small and large blebs, which rupture and
expose raw, oozing surface, and often with considerable underlying swelling of the
parts. In some instances there is a tendency to pustulation, and even sometimes to the
development of ulceration. The eruption, which is usually intensely itchy, is frequently
first observed between the toes. It may be limited to a part of one foot or may involve
both extensively; the toes and lateral parts are the favorite localities. With good man
agement the cutaneous disturbance subsides in a few weeks, but in those cases in which
scratching and secondary coccic infection occur, the eruption lasts much longer and
may extend somewhat beyond its usual regional limit, and occasionally lead to obstinate
ulcerations, and exceptionally to gangrene. It is not uncommon for a person to have
several attacks, each due to exposure to a fresh invasion of the larvæ.
The treatment of the cutaneous irritation consists in cleanliness, the use of mild
antiseptic lotions and ointments, such as are used in the acute types of eczema and
other types of acute dermatitis; the opening of vesicles, blebs, and pustules, and their
cleansing and disinfection. Long soaking of the parts in antiseptic solution, such as
boric acid solution and weak corrosive sublimate lotions, is commended. The avoid
ance of going barefooted in the warm, rainy season is a positive preventive measure.
It is thought by some observers that in some of the cases of so-called ground itch the
malady may be due to bacterial infection other than that of the hookworm larvæ.
Trypanosomiasis,1 in its advanced stages known as ‘‘sleeping sickness” results
from the invasion of the body by a minute flagellate parasite through the intermediary
of a certain insect, belonging probably to the species glossina palpalis. There is
usually a variable irritation at the points of cutaneous puncture made by the insect,
through which the trypanosome gains entrance to the body; and later at the point or
points of irritation there may arise a red or violaceous, furunculoid, slightly elevated
swelling. After several days these formations may have disappeared, leaving behind
pigmented spots which gradually fade away. In other instances the reaction may be
more intense, sometimes with markedly inflammatory symptoms and edema. Appar
ently suppuration does not occur. In these more violent cases there is considerable
constitutional disturbance, with lymphangitis and adenitis. The nucha, limbs, knees,
flanks, and axillary regions are the favorite sites. Later, when the systemic malady is
developed, the eruptive phenomena may consist of itchy vesicopapular lesions, poly
morphous urticarial erythemas, and the more or less diagnostic polymorphic erythemas,
which assume the type of erythema circinata, the ring-like patches being sometimes
several inches or more in diameter. The constitutional involvement gradually be
comes severe, anemia, nervous, and other like symptoms present, with mental and phys
ical lassitude, and the patient may succumb. The malady was for a time thought to
be more or less limited to the dark race in portions of Africa, but is now known to occur
elsewhere, and also among the whites.
In the treatment much stress has been placed on arsenic. Prophylaxis is, however,
the important part in the control of the malady, protection from insects, etc For the
cutaneous symptoms, antiparasitic and mildly antiseptic lotions may be employed when
required.
1 Some recent literature: Manson, “Tropical Diseases”; Rogers, “Fevers in the
Tropics,” 1908; and Darré, “Les symptomes cutanés de la trypanosomiase humaine,”
Annales, 1908, p. 673 (review, with many references).
But first, if you want to come back to this web site again, just add it to your bookmarks or favorites now! Then you'll find it easy!
Also, please consider sharing our helpful website with your online friends.
BELOW ARE OUR OTHER HEALTH WEB SITES: |
Copyright © 2000-present Donald Urquhart. All Rights Reserved. All universal rights reserved. Designated trademarks and brands are the property of their respective owners. Use of this Web site constitutes acceptance of our legal disclaimer. | Contact Us | Privacy Policy | About Us |